Primary objective of pulp therapy is to maintain the integrity and health of the teeth and their supporting tissues by maintaining the vitality of the pulp of a tooth affected by caries, traumatic injury or any other cause damaging the liveliness of the pulp.
Indication and the type of the pulp therapy depends on the status of the pulp, whether it’s nonvital or vital and the type of the tooth whether its primary, young permanent or permanent. Status of the pulp would be determined by clinically with a proper history and a thorough clinical examination and by accurate special investigations such as vitality testing and radiographs. In this article I would mainly consider on the treatments to the pulp in primary teeth.
Vital pulp therapy for primary teeth diagnosed with a normal pulp or reversible pulpitis
Indirect pulp treatment
A procedure performed in a tooth with a deep carious lesion approximating the pulp but without signs and symptoms of pulp degeneration. The caries surrounding the pulp is left in place to avoid pulp exposure and is covered with a biocompatible material. A radiopaque liner such as a dentin bonding agent, resin modified glass ionomer, calcium hydroxide, zinc oxide-eugenol or glass ionomer cement is placed over the remaining carious dentin to stimulate healing and repair. Then the tooth is restored with a material that seals the tooth from micro leakage.
Direct pulp treatment
When a pinpoint mechanical exposure of the pulp is encountered during cavity preparation or following a traumatic injury a biocompatible radiopaque base such as mineral trioxide aggregate (MTA) or calcium hydroxide may be placed in contact with the exposed pulp tissue. Finally the tooth should always be restored with a material that seals the tooth from micro leakage.
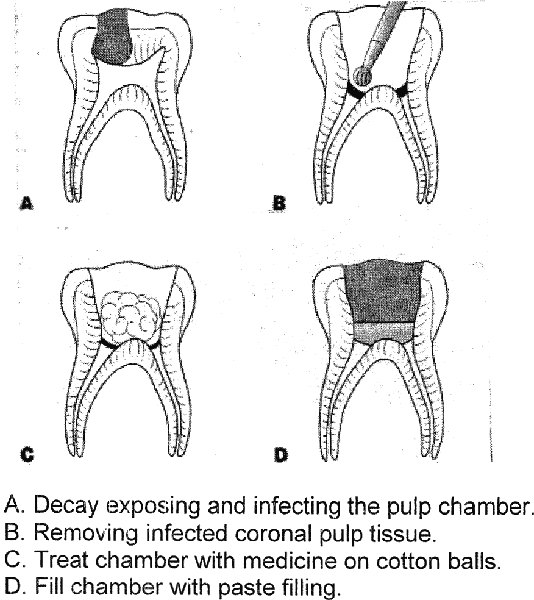
Pulpotomy
A pulpotomy is performed in a primary tooth with extensive caries but without evidence of radicular pathology when caries removal results in a carious or mechanical pulp exposure. The coronal pulpotomy is amputated and the remaining vital radicular pulp tissue surface is treated with a medicament such as Buckley’s solution of formocresol. Gluteraldehyde and calcium hydroxide have been used but with less long term success. MTA is a more recent material with a high rate of success in pulpotomies. The coronal pulp chamber can be filled with zinc-oxide eugenol or other suitable base followed by acoronal restoration to avoid micro leakage and failure of the treatment. The most effective long term restoration has been shown to be a stainless steel crown although other alternatives such as composite resin and amalgam play a role when an adequate amount of enamel is intact.
Pulpectomy
This involves the complete amputation of the pulpal tissue in a tooth that is reversibly infected or necrotic due to caries or trauma. The root canals are debrided mechanically with hand or rotary files and chemically with disinfectants such as sodium hypochlorite or chlorhexidine to ensure optimal bacterial decontamination of the canals. After proper drying of the canals a resorbable material such as non-reinforcedzinc oxide-eugenol, iodoform based paste or a combination paste of iodoform and calcium hydroxide is used to seal the canals.Then the tooth is restored with a material that seals the tooth from micro leakage.